Mental Defectives Act 1911
The Mental Defectives Act 1911 allowed people to admit themselves to mental hospitals voluntarily. This encouraged early treatment of some mental illnesses and helped reduce the stigma of committal (compulsory admission) and residence in a mental institution. The official term ‘asylum’ was replaced by ‘mental hospital’, a ‘lunatic’ became an ‘inmate’, and female ‘attendants’ became ‘mental nurses’ (male staff were still called attendants). A 1928 amendment to this Act anticipated separate training institutions for intellectually handicapped patients.
Changing the asylum model
The aim was that mental hospitals would replace the discredited asylum model by acquiring the therapeutic status and public acceptability of general hospitals. Mental hospitals facilitated easier admission procedures, active early treatment, and professional care by specialist psychiatrists and trained mental health nurses. They also provided separate ‘reception homes’ or ‘neuropathic hospitals’ for early treatment.
New Zealand psychiatry
Dr T. Gray, a young British-trained psychiatrist, described his first experience of New Zealand mental hospitals in the early 20th century: ‘The almost complete divorcement of psychiatry from general medicine created a profound impression upon me when I came to New Zealand [in 1911]. I was struck by the singularly isolated position which the mental hospitals occupied in the public life of the country … their existence was merely tolerated as a necessary evil and their drab and dreary structure and routine symbolised the hopelessly pessimistic attitude of the public towards the prognosis of those who had to be admitted.’1
The villa system
The villa system was a hospital design based on a group of small detached buildings rather than a single large and imposing structure. This design became government policy from 1903, making it much easier to classify patients by age, gender, behaviour, likelihood of recovery and, to some extent, social class. A typical self-contained 40–50-bed villa had several dormitories and single rooms, kitchen, dining room, lounge and offices. In 1969 a quarter of all mental patients were still housed in traditional asylum-era buildings. These 19th-century buildings were much harder to modernise.
The effect of shell shock
Public pressure for ‘halfway houses’ to treat nervous disorders helped take services out of mental hospitals, especially those for war veterans. Queen Mary Hospital at Hanmer Springs opened in 1916 as the first ‘halfway house’ to treat nervous breakdown, shell shock and borderline mental conditions. The treatment and status of people suffering from mental illness improved after the First World War, as numbers of shell-shocked war veterans returned to New Zealand. Patriotism demanded that these men should not be treated like ordinary mental patients, who were then widely regarded as incurable.
War veterans were treated with dignity and compassion, and gently encouraged to talk about the circumstances that had caused their illness. Because of the rapid success of this early form of psychotherapy, it was later applied to some other groups of patients in mental hospitals.
In the same period, a few doctors in general hospitals grew more interested in psychiatry (the diagnosis and treatment of mental disorders). Some hospital boards began providing observation wards for mental patients at base general hospitals, to protect ‘those of unsound mind from the indignity, distress and humiliation of being treated as delinquents and criminals’.2 Psychiatrists in mental hospitals set up outpatient clinics where they could treat less serious patients without admitting them.
New treatments
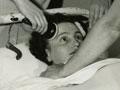
From the late 1930s a number of new treatments for severe mental illness were introduced. It was hoped that these would transform the lives of people with chronic illness. They included injecting patients to induce insulin coma and prefrontal leucotomy (a form of surgery on the brain). Both produced serious side effects and were eventually discontinued. Convulsive therapy was initially introduced using a chemical to induce a seizure but electroconvulsive therapy (ECT) soon replaced it as more reliable and safer. While considered a beneficial treatment for some, it has become increasingly controversial. Over time ECT was modified for greater safety, and it is still occasionally used.