A private professional service
Having proven their worth in wartime, raised their professional status and income and maintained a private-sector monopoly on the treatment of adult teeth, dentists consolidated control of their industry in the 1950s.
During the 1960s dentists struggled with the ‘lack of control and direction’ in the dental technicians’ industry. Legislation eventually saw the establishment of a Dental Technicians’ Board and registration for dental technicians; however, dental technicians wanted to treat patients directly, to which the New Zealand Dental Association (NZDA) was strongly-opposed.
A Royal Commission of Inquiry into Social Security in 1969–72 considered the place dentistry should occupy with in the social security system. As a result, dentists were authorised to recommend people for sickness benefits, write prescriptions, and have dental laboratory work paid for by the state. The Commission rejected a request for a universal free dental service.
A busy man
John Walsh was a vigorous and determined dean of the faculty of dentistry at the University of Otago from 1946 to 1971. He restructured the school, oversaw the building of a new Dunedin dental school in 1961, edited the New Zealand Dental Journal, designed an early (and never made) version of the high-speed dental drill, wrote three books on dentistry, and worked hard to raise awareness of dental health and make false teeth unfashionable. In August 2001 the university’s dental-school building was named the Walsh Building in his honour.
Research, specialisation and new technology
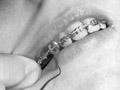
After 1946, under the vigorous leadership of the new dean, Professor John Walsh, the Otago University dental school gained an international reputation. Walsh increased emphasis on ethics, patient service and graduate research into diet and dental health. He also promoted specialisation in orthodontics (correction of teeth), gum disease, prosthodontics (the restoration and replacement of teeth), dentistry for children and dental anaesthesia.
New technology, including high-speed drills, X-rays, improved pain relief and operating chairs that allowed the dentist to sit down, helped improve the effectiveness of chair-side dentistry.
Challenges
Professional, academic and technological advancement was not matched by improvement in adult oral health. A national survey of adult oral health and attitudes to dentistry in 1976 documented the nation’s poor oral health.
During this decade, the concept of a dental team was frequently brought up by the NZDA. Adding an auxiliary to the team, in an operating (dental therapist) or preventive (dental hygienist) role, would decrease dentists’ workloads and add a preventive focus. No clear consensus on what form such an auxiliary would take led to further delays in introducing dental hygienists to New Zealand.
A second World Health Organization international oral health survey in 1988 found a much improved level of oral health in New Zealand with a low level of treatment need. Unfortunately, this and other research in the 1980s revealed another oral health issue, that of ethnic and socioeconomic inequalities in oral health between groups of New Zealanders.
In the 21st century, while most children access free dental care, the majority of adults must pay privately for dental services. A further national oral health survey in 2009 found that the main barrier to dental care for adults was cost, with more than half those surveyed reporting they did not see a dental professional often enough. The oral health of New Zealanders of all ages remains closely-related to their socio-economic status and ethnicity.