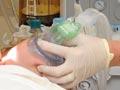
Hospital fees in the 19th century
Early public hospitals did not provide free treatment unless patients could not pay. In 1885 charitable aid boards were established to manage hospitals. Hospitals were now financed by patient fees, voluntary contributions, local rates and a government subsidy. By the late 19th century increasing staff and equipment costs meant that boards more actively sought to recover fees from patients.
Bludgers and paupers
Hospitals charged fees for social as well as economic reasons. In 1885 the inspector of hospitals, Dr G. W. Grabham, declared: ‘the provision of free hospital treatment by the Central Government is pauperising the population to an alarming extent, and taking away inducement for thrift.’1
Hospital care for Māori
The first four public hospitals, established by Governor George Grey, promised to provide free treatment for Māori. Later, authorities debated whether this was an obligation under the Treaty of Waitangi or whether only Māori who could not pay should receive free treatment. Hospitals in areas where Māori did not pay rates were reluctant to provide this service. These issues came to the fore in the 20th century as more Māori sought hospital care.
In the 19th century Maori were reluctant to go to a hospital once deaths had occurred there, as this made them tapu. Hospitals were culturally insensitive and made few allowances for extended family to stay. During the 20th century all sectors of society, including Māori, were more willing to use hospitals. This change was assisted by the Social Security Act 1938, which removed the distinction between charity cases and those able to pay for treatment.
Free hospital care
The Labour Party’s founding manifesto promised free medical treatment for all. Labour became the government in 1935 and passed the Social Security Act 1938, which promised security from the cradle to the grave. This included free treatment for all in public hospitals and 14 days free care in hospital for women following childbirth.
Private hospitals
Increasing numbers of private hospitals were established from the early 20th century. In 1908 there were 56 public hospitals in New Zealand and 191 private hospitals. Private hospitals remained an option after public hospital care became free in 1938. Most were small operations owned by doctors or midwives, and often they were little more than nursing homes for the middle class. Most were unable to compete with the high-tech equipment and range of services offered at public hospitals.
Despite this, some private hospitals flourished in subsequent decades. The introduction of private medical insurance offered by companies such as Southern Cross (started in 1961) made them attractive for those willing to pay insurance premiums. Waiting lists in public hospitals were a further incentive. The introduction of accident compensation in 1974 boosted the private sector because patients could use compensation money to pay for care in these hospitals. Some private hospitals, such as Mater Misericordiae Hospital in Auckland, grew to rival public hospitals in size and function.
Funding public hospitals
The public sector, which offered free hospital care, continued to be the mainstay of New Zealand’s hospital services. From 1957 all funds came from central government, though it had little control over how this money was spent. By the late 20th century an ageing population, new health technologies and growing consumer expectations meant that the cost of running public hospitals soared. An attempt by the government to introduce overnight charges of $50 for patients in public hospitals in 1991 met with widespread disapproval and was abandoned as an election approached in 1993. This reaction demonstrated the public’s continuing commitment to paying for public hospitals through general taxes rather than user charges.
Expensive visitors
High-tech medicine was expensive and contributed to budget blow-outs. In the 1970s there were only three public cardiac surgery units (at Green Lane, Wellington and Dunedin hospitals). About 40% of Wellington’s cardiac patients and half of the Green Lane cases came from outside their respective regions. Their costs were approximately $600 per patient per day, a figure which far exceeded the $260 per day flat rate paid to hospital boards for each outside patient in their care.
In 1983 area health boards were established to replace hospital boards. Funding was based on population size. The National government separated health providers from funders in 1993, and the area health boards were turned into Crown health enterprises (hospital and health services from 1996). These operated like businesses and competed for contracts with four separate funding agencies called regional health authorities. Many hospitals were closed during this period. A new Labour-led government (elected in 1999) replaced the regional health authorities with 21 non-profit district health boards (20 after Otago and Southland merged in 2010).
The district health boards received government funding according to a population-based formula which took into account the socio-economic status, ethnicity and age of their populations. This funding formula was updated regularly using demographic information from the latest census. In 2015/16 this formula was used to distribute $11.7 billion to health boards. In 2022 district health boards were abolished and replaced by two national organisations, Te Whatu Ora Health New Zealand and Te Aka Whai Ora Māori Health Authority. The latter was abolished in 2024.